|
|
Post by Admin on May 3, 2020 19:36:26 GMT
 COVID-19 damages the hemoglobin, impairing the ability of red blood cells to transport oxygen throughout the body, compromising the lungs and resulting in Acute Respiratory Distress Syndrome (ARDS), Italian pharmacology scholar Annalisa Chiusolo explained to The Jerusalem Post. If her thesis is correct, it would resolve many outstanding questions about the novel coronavirus, such as the greater vulnerability of men – specifically male diabetics – to become seriously ill from the virus, as well as the lower rate at which pregnant women and children contract COVID-19. Moreover, understanding this mechanism could lead the way to a quicker discovery of the most effective drugs to treat the virus. Chiusolo is a graduate of the Faculty of Pharmacy of the University of Perugia, Italy, and works as a pharmacist in the European country. Her theory has been published by some of the country’s leading newspapers, including the Italian dailies Il Tempo and Il Giornale. She told the Post that SARS-CoV-2, the formal name for the novel coronavirus, needs porphyrins for its survival – and probably for its replication – so it attacks hemoglobin, the protein that carries oxygen in the blood, which translates to less oxygen available for the body. The consequence of less oxygen is the accumulation of carbon dioxide. “The lung cells become the site of the cytokine cascade, an enormous immune response, which is responsible for the acute lung inflammation that characterizes COVID-19 pneumonia,” she said. “The value of hemoglobin in the blood can be an important parameter to assess the SARS-CoV-2 infection: In men the normal value of hemoglobin (Hb) is higher than in women. This would explain the higher incidence of COVID-19 pneumonia in men compared to women, and the lower incidence and better prognosis in children and pregnant women, where Hb values are lower due to an increased need of iron, which makes less available this ‘nutrition’ for the virus.” PNEUMONIA CAUSED by the coronavirus is also more prominent in elderly patients or middle-aged patients with diabetes, which Chiusolo said is linked to increased glycated hemoglobin. As a pharmacist, Chiusolo next evaluated the use of hydroxychloroquine to treat SARS-CoV-2, which in some cases has been found to reduce hospitalizations from the virus. Hydroxychloroquine is currently in use for the treatment of autoimmune diseases worldwide, such as lupus and rheumatoid arthritis, and has been used for years to treat malaria. She said that in addition to the drug’s antiviral and immunomodulatory effect, it binds to the ferriprotoporphyrin of the ecgonine methyl ester (EME), blocking the key enzyme of malaria. “So, I thought this same mechanism could be used against SARS-CoV-2... Indeed, a study by a Chinese university shows that SARS-CoV-2 binds to the beta chain of hemoglobin, inhibiting EME metabolism.” Ferriprotoporphyrin is the group responsible for the oxygen binding of hemoglobin. In Italy, top scientists are beginning to comment on Chiusolo’s theory. Dr. Giuseppe Ippolito, scientific director of the Lazzaro Spallanzani National Institute for Infectious Diseases in Rome, called her hypothesis, “suggestive, but it is necessary to deepen and research.” Dr. Giovanni Martinelli, scientific director at the Istituto Scientifico Romagnolo per lo Studio e la Cura dei Tumori (IRCCS), validated that “much of the effects of oxygen starvation in COVID patients may be due to the displacement of Hbs protoporphyrin.” BUT DOCTOR Amiram Goldblum, head of the Molecular Modeling and Drug Design Institute for Drug Research and the Fraunhofer Project Center for Drug Discovery and Delivery at the Hebrew University of Jerusalem, said that among the nearly 8,500 papers filed on the novel coronavirus in the last three months not one mentions porphyrin or protoporphyrin. “As far as I am aware of the reduction of oxygen pressure in severe cases of the SARS-CoV-2 attack, it is due to blocking lung cells in a somewhat similar manner as emphysema – transforming the cells to be more rigid, fibrous entities,” he told the Post after reviewing Chiusolo’s study. He said that the first FDA approved drug, Remdesivir by Gilead Pharmaceutical, is indicated only for those cases in which oxygen pressure was reduced to a more dangerous level. “If the virus ‘eats up’ the porphyrin of hemoglobin, the first effect should be anemia, which affects oxygen intake but also affects substantial weakness and is easily measured,” Goldblum said. “I have not heard of any problems with lower hemoglobin in COVID-19 patients.” |
|
|
|
Post by Admin on May 3, 2020 22:44:43 GMT
ARS-CoV-2 infection in beta thalassemia: preliminary data from the Italian experience Irene Motta1, Margherita Migone De Amicis2, Valeria Maria Pinto3, Manuela Balocco3, Filomena Longo4, Federico Bonetti5, Barbara Gianesin6, Giovanna Graziadei2, Maria Domenica Cappellini1, Lucia De Franceschi7*, Antonio Piga4*, Gian Luca Forni3 To the Editor: Patients with pre-existent chronic morbidities are likely to be more severely affected by SARS-Cov2 infection, but no data are available regarding Thalassemic Syndromes (TS). TS and hemoglobin variants represent, according to WHO, one of the most frequent causes of anemia, affecting more than 7% of the world population1. TS are classified in either transfusion-dependent thalassemia (TDT) or non-transfusion-dependent thalassemia (NTDT). Infectious complications, mainly from bacteria, constitute a common cause of mortality and morbidity in TS. Stress erythropoiesis, iron overload, splenectomy and adrenal insufficiency among others may contribute to increase susceptibility to infection2. To verify the impact of SARS-CoV-2 infection on TS, we set-up a specific survey by electronic Case Report Form (eCRF)3. Inclusion criteria require at least 15 days of follow-up from either the onset of symptoms or SARS-CoV2 positivity. The survey was approved by Ethics Committee and eCRF was shared with the Centers of Italian Hemoglobinopathies Network. The “Società Italiana Talassemie ed Emoglobinopatie” (SITE), has estimated the presence in Italy of approximately 5000 TDT and 1900 NTDT patients3. As of April 10th, 2020, 11 cases of TS and COVID-19 have been collected (See Supplementary Information). All the reported patients are in Northern Italy, where the rate of infection is higher, reflecting the national epidemiology. The mean age is 44±11 years (range 31-61 years) and 55% (6/11) are females. Ten patients are TDT, and one is NTDT. All the patients have thalassemia associated comorbidities, eight are splenectomized, and one patient (#9 in table of Supplementary Information) has pulmonary hypertension treated with sildenafil. The likely source of infection has been detected in 55% (6/11) of cases: 2 had contacts with COVID-19 positive subjects, and 4 had occupational exposure (3 are nurses working in hospital or assisted living facilities). Three patients were asymptomatic. One patient (#3 in Supplementary Information) was admitted for high fever and bone marrow hypoplasia, lymphopenia, and agranulocytosis (on treatment with deferiprone) and tested positive at the third swab. 6/11 were hospitalized, but no one required mechanical ventilation. The patient with more severe symptoms who required more intensive ventilation support with continuous positive airway pressure (CPAP) has a history of diffuse large B-cell lymphoma treated with chemotherapy in the previous year, currently in complete remission. Of the 6 admitted to the hospital, only three received supposedly specific treatment for COVID-19: one hydroxychloroquine (HCQ), one HCQ plus ritonavir/darunavir, and one HCQ plus anakinra. Patient #3 did not receive HCQ due to concomitant therapy with amiodarone and an increased risk of life-threatening arrhythmia. The clinical course ranged from 10 to 29 days. Ten patients have clinically recovered and are on a daily remote phone call follow-up. Splenectomy which was present in 8/11 patients did not seem to affect the clinical course. Of note, except for the patient with myelosuppression, no increase in blood requirement was observed. When luspatercept treatment was halted in the NTDT patient, hemoglobin fell from 11 to 8,2 g/dL, a value similar to the pre-luspatercept period. Neither death nor severe SARS or signs of cytokines storm, were observed in these 11 subjects. which may be surprising, taking into account the mean age and the presence of severe comorbidities. Our data, although preliminary, do not indicate increased severity of COVID-19 in TS. A larger number of cases needs to be collected to define the impact of this new infection and its outcome in these fragile patients. References 1. Modell B. Global epidemiology of haemoglobin disorders and derived service indicators. Bull. World Health Organ. 2008;2008(6):480–487. 2. Taher AT, Weatherall DJ, Cappellini MD. Thalassaemia. Lancet. 2018;391(10116):155–167. 3. www.site-italia.org/2020/covid-19.php. SITE communication. Accessed April 1, 2020. . |
|
|
|
Post by Admin on May 7, 2020 0:16:22 GMT
Researchers in the US and UK have identified hundreds of mutations to the virus which causes the disease Covid-19. But none has yet established what this will mean for virus spread in the population and for how effective a vaccine might be.  The question is: which of these mutations actually do anything to change the severity or infectiousness of the disease? Preliminary research from the US has suggested one particular mutation - D614G - is becoming dominant and could make the disease more infectious. It hasn't yet been reviewed by other scientists and formally published. The researchers, from the Los Alamos National Laboratory in New Mexico, have been tracking changes to the "spike" of the virus that gives it its distinctive shape, using a database called the Global Initiative on Sharing All Influenza Data (GISAID). They noted there seems to be something about this particular mutation that makes it grow more quickly - but the consequences of this are not yet clear. The research team analysed UK data from coronavirus patients in Sheffield. Although they found people with that particular mutation of the virus seemed to have a larger amount of the virus in their samples, they didn't find evidence that those people became sicker or stayed in hospital for longer. Another study from University College London (UCL) identified 198 recurring mutations to the virus. One of its authors, Professor Francois Balloux, said: "Mutations in themselves are not a bad thing and there is nothing to suggest SARS-CoV-2 is mutating faster or slower than expected. "So far, we cannot say whether SARS-CoV-2 is becoming more or less lethal and contagious." A study from the University of Glasgow, which also analysed mutations, said these changes did not amount to different strains of the virus. They concluded that only one type of the virus is currently circulating. Monitoring small changes to the structure of the virus is important in understanding the development of vaccines. Take the 'flu virus: it mutates so fast that the vaccine has to be adjusted every year to deal with the specific strain in circulation. |
|
|
|
Post by Admin on May 7, 2020 5:22:25 GMT
New research reviews the current evidence of a link between obesity and COVID-19 severity. Early data seems to suggest that people with obesity are more likely to become severely ill due to COVID-19, the disease caused by the novel coronavirus. An increasing number of reports have linked obesity to coronavirus mortality, and the Centers for Disease Control and Prevention (CDC) now list severe obesity as a risk factor for severe COVID-19. The CDC define severe obesity as having a body mass index (BMI) of 40 or above. However, it is currently unclear exactly why obesity is associated with a more dangerous form of the disease. To shed light on the situation, a team of experts in Germany, the United Kingdom, and the United States have come together to review the evidence and clarify what we know so far. Their findings are published in Nature Reviews Endocrinology.  The article summarizes the preliminary data available on obesity and COVID-19. In China, where the outbreak began, data from 383 patients showed that having obesity was associated with a 142% higher risk of developing severe pneumonia associated with COVID-19. Related News Coronavirus: How contagious are children and how sick can they get? | COVID-19 Special A larger study of over 4,000 patients with COVID-19 in New York City found that severe obesity was a major risk factor for hospitalization, second only to age. In Seattle, a study of critically ill COVID-19 patients made similar findings. This analysis found that 85% of patients with obesity required mechanical ventilation, compared to 64% of patients without the condition. Moreover, 62% of the patients with obesity died of COVID-19, compared with 36% of those without obesity. However, it is important to note that this particular study included only 24 patients, all of whom were critically ill, making it difficult to draw far-reaching conclusions from the data. 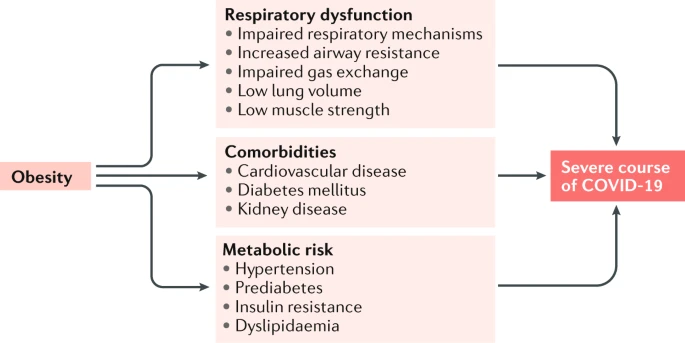 The final study included in the analysis involved 124 patients in Lille, France, and also found that patients with obesity were more likely to require invasive mechanical ventilation. Together, the evidence suggests obesity may be a significant risk factor for COVID-19. As the lead author of the study, Dr. Norbert Stefan, of the German Center for Diabetes Research, explained to Medical News Today: “We concluded that obesity may put people infected with the novel coronavirus (SARS-CoV-2) at a very high risk for a more severe COVID-19 illness and possibly risk of death.” Importantly, the risk appears to be independent of other illnesses, such as high blood pressure, that are more prevalent in people with obesity. According to the study authors, one way that obesity might increase the risk of severe COVID-19 involves respiratory dysfunction. People with obesity are more likely to have higher resistance in their airways, lower lung volumes, and weaker respiratory muscles, which are critical in the defense against COVID-19. These factors make an individual more likely to develop pneumonia, and they place additional stress on the heart. Obesity is also associated with diabetes, heart disease, and kidney disease, all of which likewise increase the risk of developing pneumonia. Setting these issues aside, high blood pressure, high cholesterol levels, and prediabetes could make people more susceptible to infection, the authors point out. The connection between the makings of diabetes and COVID-19 appears to be particularly important. “There is data emerging showing that hyperglycemia [high levels of glucose in the blood], even in the range where diabetes cannot be diagnosed, is a strong and independent predictor of a severe course of COVID-19,” explains Dr. Stefan. |
|
|
|
Post by Admin on May 8, 2020 8:05:15 GMT
The new coronavirus can persist in men's semen even after they have begun to recover, a finding that raises the possibility the virus could be sexually transmitted, Chinese researchers said Thursday.
A team at Shangqiu Municipal Hospital tested 38 male patients treated there at the height of the pandemic in China, in January and February.
About 16% of them had evidence of the coronavirus in their semen, the team reported in the journal JAMA Network Open. About a quarter of them were in the acute stage of infection and nearly 9% of them were recovering, the team reported.
"We found that SARS-CoV-2 can be present in the semen of patients with COVID-19, and SARS-CoV-2 may still be detected in the semen of recovering patients," Diangeng Li of Chinese People's Liberation Army General Hospital in Beijing and colleagues wrote.
"Even if the virus cannot replicate in the male reproductive system, it may persist, possibly resulting from the privileged immunity of testes," the team added. Privileged immunity means the immune system cannot fully reach the region to attack viral invaders.
Clinical Characteristics and Results of Semen Tests Among Men With Coronavirus Disease 2019
Diangeng Li, PhD1,2; Meiling Jin, MD2,3; Pengtao Bao, PhD4; et al
Weiguo Zhao, MD4; Shixi Zhang, MD5
JAMA Netw Open. 2020;3(5):e208292. doi:10.1001/jamanetworkopen.2020.8292
Introduction
In December 2019, an outbreak of pneumonia associated with coronavirus disease 2019 (COVID-19) occurred in Wuhan, China, and rapidly spread to other parts of China and overseas.1 It has been confirmed that COVID-19 has the characteristic of human-to-human transmission, mainly through respiratory droplets and contact. Other routes require further verification. The virus responsible for COVID-19, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been detected in stool, gastrointestinal tract, saliva, and urine samples.2 However, little is known about SARS-CoV-2 in semen.
Methods
This cohort study was performed after patients gave written informed consent for research purposes, and in compliance with the Helsinki Declaration3 with the approval of the ethics committee of Shangqiu Municipal Hospital, Shangqiu, China. This study is reported following the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guideline.
We identified all male patients with laboratory-confirmed COVID-19 aged 15 years and older between January 26, 2020, and February 16, 2020, in Shangqiu Municipal Hospital, which is the only designated hospital for the treatment of COVID-19 in Shangqiu, in the east of Henan province. Following guidance from the World Health Organization,4 laboratory confirmation for COVID-19 was defined as positive result for SARS-CoV-2 in real-time reverse transcriptase–polymerase chain reaction assay of nasal and pharyngeal swabs.1 Enrolled patients were asked to provide a semen sample for SARS-CoV-2 testing.
Groups were compared using the t test, χ2 test, or Mann-Whitney or Kruskal-Wallis test. All statistical analyses were performed using SPSS statistical software version 19 (IBM). P values were 2-tailed, and P < .05 was considered to indicate significant differences.
Results
Among 50 patients identified, 12 patients were unable to provide a semen specimen because of erectile dysfunction, being in a comatose state, or dying prior to recruitment; therefore, a total of 38 patients were enrolled for semen testing. Of these 38 participants who provided a semen specimen, 23 participants (60.5%) had achieved clinical recovery and 15 participants (39.5%) were at the acute stage of infection. Results of semen testing found that 6 patients (15.8%) had results positive for SARS-CoV-2, including 4 of 15 patients (26.7%) who were at the acute stage of infection and 2 of 23 patients (8.7%) who were recovering, which is particularly noteworthy. But there was no significant difference between negative and positive test results for patients by age, urogenital disease history, days since onset, days since hospitalization, or days since clinical recovery. The clinical characteristics of patients with positive test results for SARS-CoV-2 in semen are shown in the Table.
Discussion
In this cohort study, we found that SARS-CoV-2 can be present in the semen of patients with COVID-19, and SARS-CoV-2 may still be detected in the semen of recovering patients. Owing to the imperfect blood-testes/deferens/epididymis barriers, SARS-CoV-2 might be seeded to the male reproductive tract, especially in the presence of systemic local inflammation. Even if the virus cannot replicate in the male reproductive system, it may persist, possibly resulting from the privileged immunity of testes. So far, researchers have found 27 viruses associated with viremia in human semen. But the presence of viruses in semen may be more common than currently understood, and traditional non–sexually transmitted viruses should not be assumed to be totally absent in genital secretions.5,6 Studies on viral detection and semen persistence are beneficial to clinical practice and public health, especially concerning viruses that could cause high mortality or morbidity, such as SARS-CoV-2.
This study is limited by the small sample size and the short subsequent follow-up. Therefore, further studies are required with respect to the detailed information about virus shedding, survival time, and concentration in semen.
If it could be proved that SARS-CoV-2 can be transmitted sexually in future studies, sexual transmission might be a critical part of the prevention of transmission, especially considering the fact that SARS-CoV-2 was detected in the semen of recovering patients. Abstinence or condom use might be considered as preventive means for these patients. In addition, it is worth noting that there is a need for studies monitoring fetal development. Therefore, to avoid contact with the patient’s saliva and blood may not be enough, since the survival of SARS-CoV-2 in a recovering patient’s semen maintains the likelihood to infect others. Our study might contribute by providing new information to the current discourse regarding COVID-19 prevention and control.
|
|




