|
|
Post by Admin on Mar 24, 2020 18:40:03 GMT
Is there any way to know whether someone has had Covid-19 in the past?
Dr William Hillmann: At this point, we don’t have a test to tell that. We are developing antibody tests to check for a prior infection, but those aren’t ready for clinical use yet. The only definitive way to know that you’ve had it is to get tested while you have it and to have that test be positive.
Could I have had it and been asymptomatic?
Hillmann: Coronavirus is actually quite a significant spectrum of symptoms, from people who are entirely asymptomatic and would have no idea that they have it to people with very mild, cold-like symptoms – runny nose, congestion, sore throat – to people with more flu-like symptoms – high fevers, muscle aches, shortness of breath and cough. All the way up to people with severe illness, who we’re seeing in the hospital with respiratory failure, requiring ICU care. (Editor’s note: recent reports suggest that loss of smell and taste are also signs of Covid-19 infection.)
What percentage of carriers are asymptomatic?
Dr David Buchholz: Right now in New York, we’re only testing the sickest possible people. So we have no idea. However, there was a study in Iceland, which tested a large segment of its population, and 50% of the people who tested positive had no symptoms.
Are people who are asymptomatic also contagious?
Hillmann: A significant proportion of people who are totally asymptomatic are contagious for some portion of time. We just don’t know [for how long] at this point, because we don’t have the kind of testing available to screen for asymptomatic infections.
When people are symptomatic, they’re contagious. A day or two before they become symptomatic, they’re likely contagious as well. A virus builds up and starts to shed, and then after symptoms resolve, people can still be contagious for a couple of days. We have some evidence of viral shed even a couple of weeks after symptoms are resolved. It’s hard to know if that’s actual live virus, which is still able to infect somebody, or if that’s just dead virus that the body is shedding.
Should someone behave differently if they think, but don’t know for certain, that they have already had it?
Buchholz: We all have to be role models. If we’re all in it together, we all should be doing social distancing.
Hillmann: Since there’s no real way to know at this point who might have had it, unless you’re symptomatic, you get a swab and are definitively diagnosed with it, I would just act as if you hadn’t had it. Keep doing all of those things that we all should be doing at this point: social distancing and hand hygiene.
If I think I may have had it, do I have an ethical obligation to tell people I came in contact with? Even if it may in fact just have been a cold?
Buchholz: I would, absolutely. I’m in New York, and it was definitely in the community before we knew it. So, yeah, any family members and close friends, maybe somebody you work next to, I think I would just alert them, especially if it was in the last 14 days. If it’s been more than 14 days, they would have gotten sick by now if they had significant exposure.
Hillmann: It’s up to every individual about what they feel is right. If somebody is diagnosed with a case of coronavirus, I might feel a little bit more strongly that they should tell people because if you’re in close contact with a healthcare worker, it could have implications for precautions that healthcare worker needs to take.
If I’ve had it, can I get it again?
Buchholz: There’s not been any evidence that anyone’s gotten it more than once. Someone with a normal immune system that can react to the virus and get better should have immunity for quite some time, at least a year, if not lifelong.
Experts
Dr David Buchholz, senior founding medical director, primary care, assistant professor of pediatrics, Columbia University Irving medical center
Dr William Hillmann, associate inpatient physician director at Massachusetts general hospital
|
|
|
|
Post by Admin on Mar 26, 2020 1:30:34 GMT
New York City Mayor Bill de Blasio plans to hold a press conference on the coronavirus outbreak that has infected more than 14,900 people in the city.
Earlier on Tuesday, New York Gov. Andrew Cuomo said a "troubling and astronomical" number of coronavirus cases has increased the urgency across the state for more hospital beds as the outbreak spreads "unabated." Cuomo was speaking at the Jacob K. Javits Convention Center in New York City, where the Army Corps of Engineers is building four FEMA hospitals with 250 beds each for coronavirus patients.
On Friday, de Blasio said New York City had become the epicenter for the coronavirus outbreak in the nation. At that point the city had a third of all coronavirus cases in the nation. He also warned that the city will run out of protective gear for medical workers in two or three weeks if cases keep rising at this rate.
"If you feel afraid, you are not alone, if you're anxious you are not alone," de Blasio said. "New Yorkers are so strong. There are other places in this country this might be a particularly shock to the system, but here ... we are tough people by nature."
The coronavirus has infected at least 46,500 people in the U.S. and had killed at least 590 people, according to Johns Hopkins University data.
|
|
|
|
Post by Admin on Mar 26, 2020 5:21:59 GMT
There is a strong chance the new coronavirus could return in seasonal cycles, a senior US scientist said Wednesday, underscoring the urgent need to find a vaccine and effective treatments.
Anthony Fauci, who leads research into infectious diseases at the National Institutes of Health, told a briefing the virus was beginning to take root in the southern hemisphere, where winter is on its way.
"What we're starting to see now... in southern Africa and in the southern hemisphere countries, is that we're having cases that are appearing as they go into their winter season," he said.
"And if, in fact, they have a substantial outbreak, it will be inevitable that we need to be prepared that we'll get a cycle around the second time.
"It totally emphasizes the need to do what we're doing in developing a vaccine, testing it quickly and trying to get it ready so that we'll have a vaccine available for that next cycle."
There are currently two vaccines that have entered human trials -- one in the US and one in China -- and they could be a year to a year-and-a-half away from deployment.
Treatments are also being investigated -- some new drugs and others that have been repurposed, including the antimalarials chloroquine and hydroxychloroquine.
"I know we'll be successful in putting this down now, but we really need to be prepared for another cycle," Fauci concluded.
Fauci's comments suggesting the virus does better in colder weather than it does in hot and humid conditions follows a recent Chinese research paper -- still preliminary and awaiting peer-review -- that reached the same conclusion.
The reasons are thought to include that respiratory droplets remain airborne for longer in colder weather, and that cold weather weakens immunity.
Another potential reason is that viruses degrade more quickly on hotter surfaces, possibly because a protective layer of fat that envelops them dries out quicker.
But reduced infection rate does not mean the virus gets eliminated -- Australia has had almost 2,500 confirmed cases and 8 deaths, for example.
|
|
|
|
Post by Admin on Mar 26, 2020 23:38:40 GMT
As indicated by the graph by Statista below, according to Johns Hopkins University, since the pandemic started in China late last year there have been more than 487,000 confirmed cases of COVID-19. Almost 118,000 people have recovered, and 22,030 people have died. 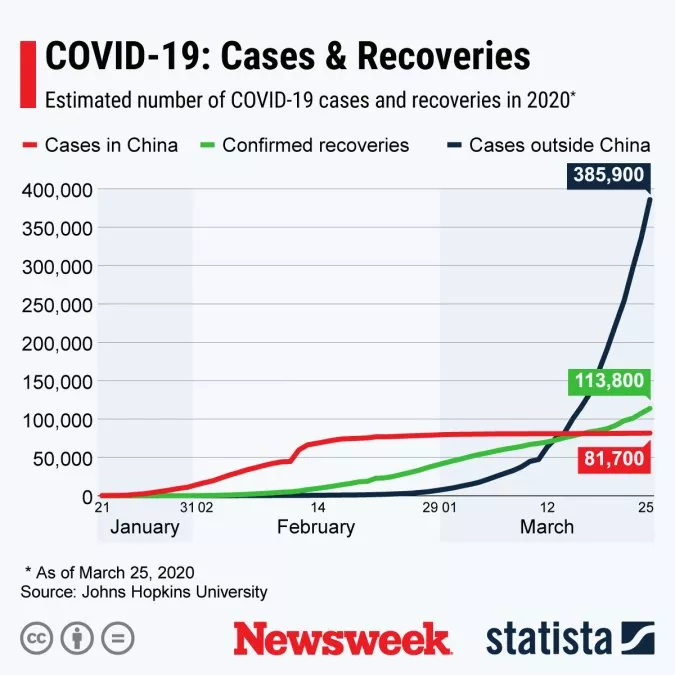 The U.S. Centers for Disease Control and Prevention (CDC) states those who are or think they are sick with COVID-19 should stay home for at least 7 days after their symptoms first appear, and call their doctor before seeking medical care. The World Health Organization (WHO) previously asked those who have been to areas where COVID-19 is spreading to self-isolate by staying at home if they start to feel unwell, "even with mild symptoms." According to the UN agency, around 14 percent of people who catch the new coronavirus will develop a severe case of COVID-19, for which they will need hospitalization and oxygen support, and a further 5 percent will need to be treated in an intensive care unit. The CDC urges those who develop the more serious symptoms of COVID-19 to seek medical attention immediately. These include: trouble breathing; persistent pain or pressure in the chest; new confusion or inability to arouse; and bluish lips or face. But as many as 80 percent of COVID-19 patients will experience a mild illness they can manage themselves at home. So how can a person tell if they've fallen ill with a mild case? A report of the WHO-China Joint Mission on COVID-19 submitted on February 28 detailed the symptoms of 55,924 people confirmed to have the disease. The patients were aged between 30 to 69-years-old, and 51 on average. 87.9 percent had a fever 67.7 percent had a dry cough 38.1 percent felt fatigued 33.4 percent produced sputum 18.6 percent had shortness of breath 13.9 percent had a sore throat 13.6 percent had a headache 14.8 percent had muscle and or joint pain 11.4 percent had chills 5 percent were sick or felt nauseous 4.8 percent experienced nasal congestion 3.7 percent had diarrhea 0.9 percent coughed up blood 0.8 percent had conjunctival congestion, or pink eye |
|
|
|
Post by Admin on Mar 28, 2020 18:13:14 GMT
The new coronavirus continues its spread in nearly every nation, bringing illness or death to many thousands of people. In the United States, the number of cases is growing rapidly. Here we ask experts questions from readers and listeners about COVID-19, and how to prevent the spread of the virus.
I know the virus can live on hard surfaces. What about clothing?
It probably can — but you shouldn't be overly worried. Here's why.
So far, there aren't scientific findings on how long the virus can live on fabric. But fabrics are generally porous — as is cardboard, which has been tested. And a recent study did find that the virus can live on cardboard for up to 24 hours.
"The thing that you have to consider, though, is that those tests are done in ideal testing circumstances," says Rachel Graham, a virologist at the University of North Carolina. "That's like in some kind of hermetically-sealed box where there's no fluctuation in humidity, there's no wind, there's nothing that can contribute toward desiccating the virus. And so desiccation — or drying out the virus — would actually reduce the amount of time it's actually viable on any kind of surface."
Plus, porousness is a good thing when it comes to virus. A surface that is permeable, like a fabric, tends to trap viruses more easily than hard surfaces.
"It's less at risk of transmitting because the virus gets kind of stuck to the [porous] surface, and so it can't be easily transferred back off of it," Graham says. "Porous surfaces also suck the fluid out of it. The viral membrane is a lipid membrane and so if that becomes dried out, it's basically done, infectivity-wise."
If you are concerned that clothing or other fabric items might have picked up the virus, throw the clothing in the washer and dryer. For most situations, says Graham, your detergent will do its job and get rid of any infective particles – or at least sanitize them to the point where they're not a risk to you.
If you're taking care of someone who is ill, immuno-compromised or you're working in a health-care setting, you may want to take additional precautions. The Centers for Disease Control and Prevention has recommendations for households with suspected or confirmed cases of the coronavirus, which include wearing gloves when handling dirty laundry from an ill person and using the warmest appropriate water setting when washing clothes or linens to disinfect them.
I like to use wipes to disinfect surfaces in my home — especially surfaces that are frequently touched. But how much surface area can one wipe be used on before it loses its ability to kill the coronavirus?
The first step is to check the label on the wipes you're using. For instance, the label on a container of Clorox wipes instructs: "Use enough wipes for treated surface to remain visibly wet for 4 minutes. To kill viruses, let stand 15 seconds."
That time and that visible wetness is important, says Erica Hartman, an expert in environmental microbiology at the Northwestern University McCormick School of Engineering.
Regardless of the particular ingredients in the wipes you're using, "they're all chemicals that have to react," she says. "And those chemical reactions aren't instantaneous — they take a certain amount of time. So what you're doing when you're keeping the surface wet is you're basically allowing time, allowing the chemical reactions to take place."
So if that Clorox wipe isn't making the surface visibly wet for 4 minutes, you're trying to cover too much ground with one wipe.
There's no exact figure for how much surface area a wipe can handle. But a 2018 study that found one wipe is generally more effective over 1 to 2 square feet than 8 square feet.
And you don't need a pre-made wipe to clean surfaces: You can also use a liquid product on a cloth or paper towel. The Centers for Disease Control and Prevention advises using products that that contain bleach (sodium hypochlorite) or alcohol (at least 70%), and following the manufacturer's directions. You can make your own cleaning solution by mixing 4 teaspoons bleach per quart of water, according to the CDC.
The U.S. Environmental Protection Agency has posted a list of approved products to disinfect against the coronavirus.
Strangers keep petting my dog when we go for a walk. Could my dog transmit the virus on its fur?
Saskia Popescu, an infection prevention epidemiologist at the health-care system Honor Health, says she's not especially concerned about dog fur transmitting the virus. "I think that I would probably be more worried if somebody was coughing all over the place and went to touch my dog's harness or something — something inanimate," she says. "I would put it in the lower risk category."
That's because like fabric, fur is a porous surface — so it isn't easy for a person to pick up bits of virus from it. "The chances of you getting it from fur and hair is going to be less than getting it from a solid surface," says virologist Rachel Graham. Still, she said, she would err on the side of caution and ask people not to pet your dog right now.
Graham says one way to make sure your dog doesn't get touched by over-enthusiastic petters is to avoid letting your dog off-leash in a place where it may encounter other people. Rather than going to a dog park, she says, "it might be a better idea to take your dog out in the yard or somewhere you know that there's not going to be a lot of people."
And despite the occasional press report of a dog diagnosed with COVID-19, there is no evidence that pets can contract or spread COVID-19. The CDC says it has not received any reports of pets or animals becoming sick with the disease. The American Veterinary Medical Association (AVMA) concurs: "Infectious disease experts and multiple international and domestic human and animal health organizations agree there is no evidence at this point to indicate that pets become ill with COVID-19 or that they spread it to other animals, including people.
One note: If you are already sick with COVID-19, AVMA recommends limiting contact with animals "out of an abundance of caution" until more is known about the virus. If you're not sick with the coronavirus, the group says you can interact with your pet as you normally would, practicing good hygiene — including washing your hands before and after interacting with your pet.
Can you get COVID-19 more than once?
The short answer: We don't know yet. It's not yet clear whether people can be reinfected by this coronavirus or how long immunity might last after infection.
Immunity after recovery from COVID-19 would be a boon in the global fight to rein in the virus. People who have recovered and gained immunity would be especially valuable as health-care workers. The spread of the virus would slow if there were fewer people. And antibodies from recovered people could help in developing a treatment for the disease.
As NPR's Nell Greenfieldboyce has reported, scientists are looking for clues about immunity and re-infection from other coronaviruses.
The severe coronaviruses SARS and MERS did produce antibodies in those who had had the virus. In the case of MERS, survivors generated an immune response to the virus that could be detected up to two years later. And the sicker the patient was, the more long-lasting their immune response.
But in the case of the four seasonal coronaviruses that are a cause of the common cold, they can sicken people over and over again. After infection with one of these viruses, antibodies are produced — but then the levels slowly decline, and people become susceptible again.
There are some indications that the new coronavirus, officially known as SARS-CoV-2, can spur immunity. New, not-yet-peer-reviewed research in rhesus macaques found that the new coronavirus does not cause reinfections.
"I think there's a very likely scenario where the virus comes through this year, and everyone gets some level of immunity to it, and if it comes back again, we will be protected from it," Matt Frieman, a coronavirus researcher at the University of Maryland School of Medicine in Baltimore, told NPR. "Either completely or if you do get reinfected later, a year from now, then you have much less disease."
"That is the hope," he adds. "But there is no way to know that."
|
|

